This sentiment remains deeply relevant today. Over the years, several key principles have emerged in the hypospadias literature, and staying abreast of these outcomes is essential. Our understanding of hypospadias has evolved from rigid dogma to nuanced decision-making. This shift is perhaps most evident in our approach to pre-operative optimization. What was once applied routinely is now guided by careful patient selection and a deeper understanding of tissue biology.
Hormonal Preparation: When and Why, It Matters
Due to potential ill effects on wound healing, routine testosterone use is no longer recommended for all cases. However, for patients with a small glans (diameter <14 mm) or a small phallus, pre-operative testosterone (2 mg/kg IM) is increasingly adopted to improve tissue vascularity and glans width, which in turn reduces the risk of glans dehiscence. In proximal cases or among testosterone non-responders, dihydrotestosterone (DHT) gel has proven extremely useful. Beyond preparation, the operative strategy itself must be guided by a careful assessment of anatomy.
Let the Anatomy Guide the Repair
The intraoperative measurement of glans and urethral plate width has become routine. In patients with a deep glans groove and a urethral plate width >10 mm at the glans hillocks, a simple Duplay repair yields excellent results. For those with a borderline urethral plate width (8–10 mm, the Tubularized Incised Plate (TIP) repair remains a reliable choice. Foreskin reconstruction is now feasible in 30–50% of cases; it is often preferable, as the preserved tissue can be utilized if complications arise. However, not all cases present with ideal anatomy, and the surgeon must be prepared to
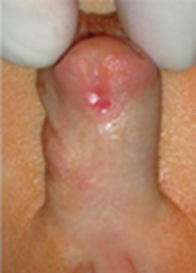
When the Plate is Not Ideal: The Value of Flaps
Mastery of flap repairs—such as the Mathieu, On-lay, and LABO for re-operative cases—is an essential skill set that can “bail out” a surgeon when the glans or urethral plate is narrow (<7mm). In parallel with urethral reconstruction, attention to penile curvature remains equally important.
Addressing Curvature: A Critical Step
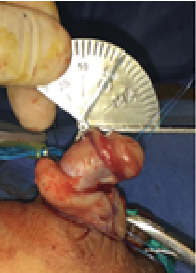
Refinements in Post-operative Care
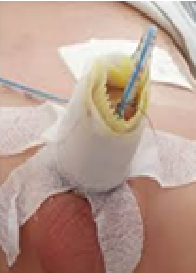
Technique Matters: Respecting Tissue
Respecting tissue planes and maintaining vascularity of outer skin are crucial steps for any type of hypospadias repair. The adoption of fine suture materials, such as 7-0 PDS or Vicryl, alongside 2.5x magnification, has significantly improved hypospadias outcomes over the years. Yet, beyond techniques and protocols lies a more personal challenge for the surgeonThe “Fear Zone” and the Young Surgeon


0 Comments